Prescription Drugs Are the Leading Cause of Death
from The Brownstone Institute by Dr. Peter Gotzsche, co-founder of the Cochrane Collaboration.
From the Brownstone Institute
Summary:
Prescription Drugs Are the Leading Cause of Death
And psychiatric drugs are the third leading cause of death
"Prescription Drugs Are the Leading Cause of Death" by Peter C. Gøtzsche discusses the significant impact of prescription and psychiatric drugs on mortality rates. Gøtzsche argues that these drugs are among the leading causes of death, surpassing many other common causes. He highlights several issues contributing to this problem:
Underestimation of Drug-Related Deaths: Many deaths caused by drugs are not recorded accurately, as they often occur outside hospitals and are not always directly linked to drug use in medical reports.
Psychiatric Drugs: Gøtzsche points out that psychiatric drugs, including antidepressants and neuroleptics, are particularly lethal. He cites studies showing high mortality rates associated with their use, especially among the elderly and those with conditions like Alzheimer’s disease.
Polypharmacy: The use of multiple drugs simultaneously increases the risk of adverse effects and death. This is common in psychiatric treatments, where patients may be prescribed several potent drugs.
Flawed Research and Regulation: The author criticises the pharmaceutical industry and regulatory bodies for not addressing the risks associated with these drugs adequately. He suggests that many clinical trials are biased and do not reflect the real-world dangers of these medications.
Over-Prescription and Misclassification: Gøtzsche argues that many drug-related deaths are preventable, as they result from over-prescription and incorrect classification of deaths. For example, deaths from falls induced by drug-induced dizziness or confusion are not always linked directly to the drugs involved.
Economic and Social Impact: The text also touches on the broader economic and social impacts of high prescription drug use, including the burden on healthcare systems and the influence of pharmaceutical companies on medical practices.
Overall, Gøtzsche advocates for a more conservative approach to drug prescription, better regulation, and more transparent and unbiased research to reduce the mortality associated with prescription and psychiatric drugs.
COMMENT:
Psychiatry is a non-scientific medical discipline. Psychiatric patients have major underlying evidence-based nutritional and toxicity conditions that are rarely if ever addressed by their GPs and psychiatrists.
Nutritional Medicine: A Comprehensive Overview
Nutritional medicine is a branch of medicine that focuses on the interplay between nutrition and the body's health, emphasising the use of food and supplements to improve health and treat diseases. This field is grounded in the fact that virtually all medical conditions and symptoms can be alleviated or even resolved through changes in diet and nutritional interventions.
Definition and Principles of Nutritional Medicine
Nutritional medicine considers how nutrients and other food components influence the function of the body, protect against disease, restore health, and influence our health status and risk of disease. It is characterised by a holistic approach, often integrating traditional food knowledge with modern scientific research to create personalised treatment plans for individuals 1 2 8.
Dietary Interventions
The cornerstone of nutritional medicine is dietary intervention, which involves tailoring the diet to meet the individual's specific health needs. This can include the adjustment of macronutrient composition, caloric intake, and inclusion or exclusion of certain food types based on the patient's condition 8.
Elimination Diets
Elimination diets are used to identify foods that an individual may be sensitive or allergic to. This involves removing certain foods or food groups from the diet for a period, then systematically reintroducing them to observe potential adverse reactions. Conditions such as irritable bowel syndrome (IBS), allergies, and skin conditions like eczema often benefit from this approach 4 1 9.
Detoxification and Toxins in Foods
Detoxification diets are designed to eliminate toxins from the body, with a focus on foods that support liver and kidney function. Awareness of natural toxins in foods, such as solanines in nightshades or mycotoxins in mouldy grains, is also crucial in nutritional medicine to prevent adverse health effects 1 7.
Nutritional Deficiencies and Their Management
Nutritional deficiencies occur when the body does not get enough of the nutrients it needs. Common deficiencies include iron, vitamin D, vitamin B12, and iodine, each associated with specific health issues such as anemia, bone weakness, neurological disturbances, and thyroid dysfunction. Addressing these deficiencies is often through dietary adjustments and supplementation3 11 6.
Nutritional Supplementation and Therapies
Megavitamin Therapies
Megavitamin therapy involves the use of large doses of vitamins, far exceeding the recommended dietary allowances, to treat or prevent diseases. This approach is based on the premise that some diseases result from vitamin deficiencies or high dose vitamin dependencies and that large doses can correct these deficiencies or exert other beneficial effects10.
Mineral Therapies
Similar to megavitamin therapy, mineral therapies involve the supplementation of minerals such as magnesium, zinc, and selenium, which play critical roles in various bodily functions. These therapies aim to correct deficiencies and support processes such as immune function, wound healing, and hormone production 10.
The Australasian College of Nutritional and Environmental Medicine
The Australasian College of Nutritional and Environmental Medicine (ACNEM) is a leading body in the field, providing training and resources for practitioners. It promotes the use of nutritional and environmental medicine practices to prevent and manage chronic diseases, emphasising the importance of diet and environment in health 9.
Application of Nutritional Medicine
Nutritional medicine is applied in various medical fields, from preventive health and chronic disease management to the treatment of acute conditions. It is particularly effective in managing lifestyle-related diseases such as diabetes, cardiovascular diseases, cancer, autoimmune diseases, psychiatric disturbances and obesity, where dietary and lifestyle changes can significantly impact the patient's health. Most importantly, it can prevent infectious diseases and their sequelae 8 12.
Subspecialty of Nutritional Psychiatry
Nutritional psychiatry is a subspecialty that explores the role of nutrition in mental health. It studies how dietary changes can affect mood, behavior, and cognition. Research in this field has shown that diets high in fruits, vegetables, unprocessed grains, and fish can improve mental health outcomes, while diets high in processed and high-sugar foods can worsen symptoms of depression and anxiety8. Fasting therapies are also effective in psychiatry. 9
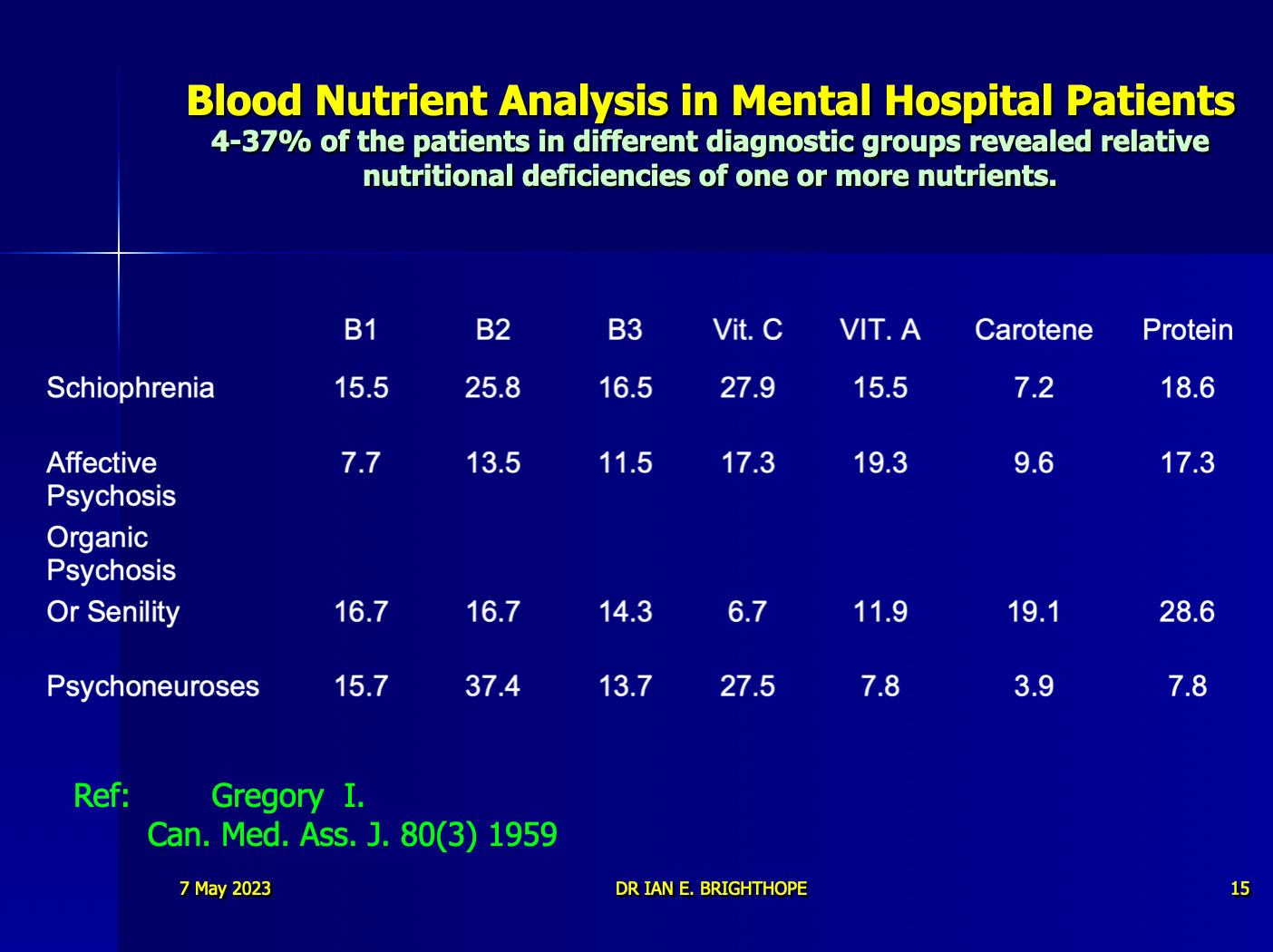
A few PowerPoint slides from my old lectures
My message here is that there is a mass of evidence going back decades supporting the cause of malnutrition in the broadest sense as a cause of mental illness.
In summary, nutritional medicine leverages the therapeutic potential of food and supplements to support and enhance various aspects of health, from immune function and digestive health to mental well-being and chronic disease management.
By integrating dietary modifications, supplementation, and an understanding of the body's nutritional needs, practitioners of nutritional medicine can significantly influence the health outcomes of their patients, providing a powerful tool for both preventive health and disease management.
See: Root cause analysis in an unscientific discipline, psychiatry, in which even common sense does not apply.
Ian Brighthope








Ian,
100 %.
When my brother died suddenly at age 44, I was 33. Mainstream medicine hospitalised me and tranquilized me and sentenced me to a lifetime of dependence on pharmaceutical drugs.
When my weight ballooned over 100 kg, I said enough.
My psychiatrist at the time smiled at me and stated I'd be on these drugs for the rest of my (shortened) life.
I called bullshit and was harshly viewed by my family.
I quit Olanzapine after towing the corporate line for over a decade and find myself at 56, fitter stronger and healthier weighing 77 kg thanks to the brave and relentless work of 'real doctors ' like you.
Rock on!🎸
There is also the growing number of victims who have been killed by people taking psychiatric drugs.